
Opinion: Why Canada’s health Innovation bottleneck is adoption, not invention
How the Waterloo Region’s health-technology ecosystem is fixing innovation

How the Waterloo Region’s health-technology ecosystem is fixing innovation
By Moazam Khan and Elliot Fung Velocity Health & Medical Innovation XchangeA portion of this opinion piece was published across Metroland newspapers (subscription required) on Wednesday April 22, 2026.
Canada does not suffer from a shortage of health innovation. It suffers from a shortage of adoption.
In a publicly funded health system under sustained strain, this gap is no longer theoretical. It affects patient access, outcomes and wait times, and limits Canada’s ability to turn world‑class research into real‑world care.
Across the country, entrepreneurs, universities and hospitals generate breakthroughs in imaging, artificial intelligence, biosensing and medical devices. Yet many of these innovations struggle to progress beyond pilots or early validation before reaching hospitals, doctors’ offices or the patient bedside. Numerous reports and founder experiences point to a common pattern: promising technologies encounter delays navigating clinical access, procurement and reimbursement before they can be deployed at scale. The problem is not a lack of ideas or talent. It is the absence of reliable pathways that move solutions from invention into everyday clinical use.
Evidence increasingly shows this gap can be narrowed when clinical access, early capital and commercialization support are deliberately coordinated, rather than left to individual founders to navigate alone.

In recent years, Ontario‑based founders supported through the Waterloo Region health‑innovation ecosystem, powered largely by the University of Waterloo’s Velocity incubator and the Medical Innovation Xchange, have contributed to improved care for more than 350,000 patients. More than 165 health‑technology companies have been supported across stages, generating roughly $200 million in revenue, creating and maintaining more than 1,300 jobs and raising more than $350 million in follow‑on capital. Together, they have filed 650 patents and counting, strengthening Canada’s innovation economy.
These outcomes matter because they reflect technologies moving beyond promise toward real clinical use.
That progress did not come from launching another accelerator. It came from reducing friction between innovation and adoption.
That friction is structural. Regulators rightly require proof of safety and effectiveness. Hospitals must manage clinical risk under tight budgets. Procurement systems are cautious by design. Yet early‑stage companies are often asked to demonstrate clinical value before they have access to trial sites, implementation partners or the capital needed to generate that evidence.
Canadian inventions often find early success in the U.S. or overseas, where incentives more clearly reward patient outcomes. Canada’s procurement and funding structures make widespread domestic adoption difficult. Without change, wait times will continue to increase, patient outcomes may suffer and system costs will rise.
The result is a familiar loop.
Without pilots, there is no data. Without data, there is no adoption. Many promising technologies remain stuck or leave the country altogether.
Ecosystems designed to break this cycle are becoming essential health infrastructure.
Backed in part by FedDev Ontario and the City of Kitchener, Velocity Health was built for this purpose. Developed with partners across Ontario and beyond, including Grand River Hospital Foundation, McMaster University, Western University, MaRS and the Medical Innovation Xchange, it provides founders with coordinated access to clinicians, clinical trial pathways and commercialization support. The Medical Innovation Xchange then supports companies as they scale, hire and manufacture in Ontario.

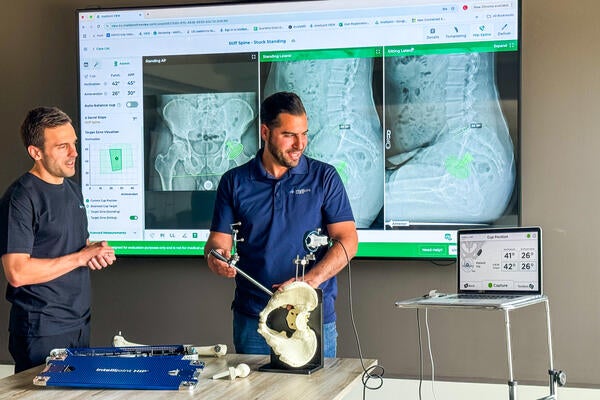
When this approach works, the results are tangible. Here are three companies founded by University of Waterloo alumni that are emerging through this ecosystem: Vena Medical has developed the world’s smallest intravascular camera and secured Health Canada licensing, along with provincial support to establish advanced manufacturing in Kitchener. Intellijoint Surgical’s orthopaedic navigation technology is now used in tens of thousands of joint‑replacement procedures worldwide. Foqus is developing MRI technologies that dramatically reduce scan times, improving patient throughput and easing bottlenecks.

Founders do not need more programming. They need systems that work.
That means clear clinical entry points, procurement models that reward outcomes, and early‑stage, public‑private capital that accelerates validation rather than backfilling late‑stage risk.
Canada can improve innovation adoption without sacrificing fiscal discipline or public health‑care values. The answer is not to slow down, but to build ecosystems that move technologies from first prototype to first clinical deployment.
The results are already visible. And they are being built in Waterloo.
Moazam Khan is Managing Director, Venture Scale and Strategy at Velocity. Elliot Fung is Executive Director at the Medical Innovation Xchange. Both work with founders to accelerate the clinical adoption of health technologies.

Read more
New initiative linked to the Velocity entrepreneurship ecosystem to support health-tech startups
Read more
Two University of Waterloo affiliated health-tech companies secure major provincial investment to bring lifesaving innovations to market

Read more
Velocity has launched a second venture capital fund targeted specifically at early-stage startups involved in health technology
The University of Waterloo acknowledges that much of our work takes place on the traditional territory of the Neutral, Anishinaabeg, and Haudenosaunee peoples. Our main campus is situated on the Haldimand Tract, the land granted to the Six Nations that includes six miles on each side of the Grand River. Our active work toward reconciliation takes place across our campuses through research, learning, teaching, and community building, and is co-ordinated within the Office of Indigenous Relations.