
Five valuable insights from a global health expert
Rohit Ramchandani (BSc ’04) shares valuable insights about COVID-19 and what the future holds

Rohit Ramchandani (BSc ’04) shares valuable insights about COVID-19 and what the future holds
By Megan Vander Woude Office of Advancement Dr. Rohit Ramchandani (BSc ’04) is the founder & CEO at Antara Global Health Advisors, a global consultancy that provides technical expertise & evidence-based public health and management advice to public and private organizations around the world. Rohit is also an Adjunct Assistant Professor in our School of Public Health & Health Systems, and co-Chair of Waterloo’s Toronto Alumni Chapter, our largest global alumni chapter, with over 50,000 alumni.
Dr. Rohit Ramchandani (BSc ’04) is the founder & CEO at Antara Global Health Advisors, a global consultancy that provides technical expertise & evidence-based public health and management advice to public and private organizations around the world. Rohit is also an Adjunct Assistant Professor in our School of Public Health & Health Systems, and co-Chair of Waterloo’s Toronto Alumni Chapter, our largest global alumni chapter, with over 50,000 alumni.
We were excited to have Rohit join us for a video chat and webcast to answer some of the hard hitting questions surrounding COVID-19. Read on to see five of the valuable insights he shared about the COVID-19 virus, how we can get back to “new-normal” life and the role we can all play in preventing pandemics.
The bottom line: COVID-19 is more infectious and more deadly than the influenza viruses we see year-over-year.
First, Rohit points to an important difference in the reproduction rates of influenza and COVID-19. Reproduction rate measures the average number of people infected by one earlier infected person in a susceptible population.
The reproduction rate of the common flu is about 1.3. If you have the flu, on average you’ll pass it on to 1.3 people, and each of them will pass it on to 1.3 people as well. After this has happened 10 times, you would be responsible for about 14 cases of the flu.
COVID-19 has a much higher reproduction rate, sitting somewhere between two and three. Some studies suggest it could be even higher. If you were to pass COVID-19 on to three people, and each of them passes it on to three more, thousands will be infected quickly. After the same 10 cycles of spread, one person would be responsible for about 59,000 cases.
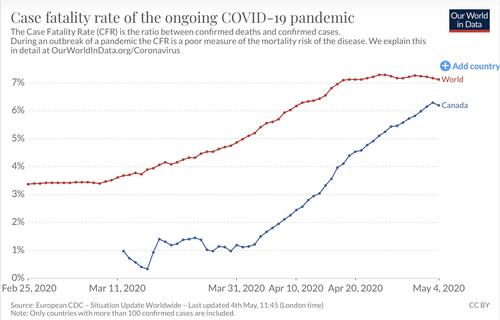
Source: Our World In Data
Given today’s data, COVID-19 also has a higher case fatality rate – the number of reported deaths divided by the number of diagnosed cases. Seasonal flu viruses tend to have a fatality rate below 0.1. COVID-19’s case fatality rate has varied across countries, but globally has ranged between three and seven. As the pandemic continues, the fatality rate will continue to shift because the number of cases and deaths will rise. With the current data, this is our best estimate, and it confirms the deadly nature of COVID-19.
“There’s really no path to ending a pandemic other than a vaccine,” explains Rohit.
According to current estimates, we could have a vaccine in 18-24 months, and that’s a much faster timeline than your average vaccine. Most vaccines take more than five years to develop and manufacture. There are multiple steps of development, testing and approvals before companies can begin to manufacture the doses that will be provided to a population.
DR. ROHIT RAMCHANDANI
The fact is that while treatments save lives, vaccines save populations.
“Developing a vaccine for COVID in 12-18 months or 18-24 months – which we believe is doable – would be a historic event in a number of ways,” says Rohit. “Many of these vaccine approaches will fail because they won’t create a strong enough immune response to provide protection, particularly in older people whose immune systems typically don’t respond as well to vaccines. And so a number of candidates need to be funded so we can advance at full speed […] and maximize the chance of finding a vaccine that works.”
As we wait for a viable vaccine, there are a lot of steps we can take to get COVID-19 under control and get back to a modified version of “normal” life. For now, physical distancing, testing, contact tracing and isolating cases are key to taming the spread of the virus.
“Once the reproduction rate is below one, we must aggressively focus on testing, contract tracing and isolation,” says Rohit.
These steps will help us gain more accurate knowledge about the spread of COVID-19 and the health of our population. It will give us a better understanding of how many people have contracted the virus and where they came in contact with it, and ensure they take the quarantine precautions seriously. Then governments can begin to lighten restrictions to take steps back to a more familiar life.
“It’s going to be something we have to take baby steps with,” explains Rohit, “and that’s really reflected in the staged approach we’re seeing released in various localities.”
To begin, we’ll see services and businesses open in a way that still allows for physical distancing and self-isolation for those who experience symptoms. For example, some businesses may be able to open, but only allow curbside pickup and delivery. Remote work arrangements will continue where possible, and it will likely be months before we see any large gatherings like concerts.
“You can’t have a healthy economy without a healthy workforce,” says Rohit.
This is a scary time – and not just for our health. Millions of individuals and businesses have been financially affected by the pandemic. While we all have a strong desire to get back to work, evidence tells us that, in the long term, it’s best for the economy if we control the spread of COVID-19 now.
According to Rohit, one of the most important things you can take from this experience is the role you play as an individual. There are many things we can all do to prevent another pandemic.
“I think it really comes down to living more conscientiously, and thinking about how our individual actions can impact the whole of society,” he says. “Educating ourselves and understanding the broader connections between our individual actions and the overall wellbeing of the planet is critical.”
These actions can be small, like proper handwashing and staying home when you and your children are sick. But for those looking for more, there are certain lifestyle and political decisions that can contribute, like eating less meat and electing leaders who will support universal health care and coverage.
Dr. Rohit Ramchandani (BSc ’04) is the founder & CEO at Antara Global Health Advisors, a global consultancy that provides technical expertise and evidence-based public health & management advice to public and private organizations around the world. He is an adjunct assistant professor in the School of Public Health & Health Systems at Waterloo, where he teaches Global Health Innovation, and was recently made a Fellow of the Balsillie School of International Affairs. As Public Health Advisor & Principal Investigator at ColaLife, he has worked around the world to help curb epidemics of diarrheal disease, the second leading cause of death in children under five globally. He sits on the Board of Directors of the Jane Goodall Institute of Canada, working on conservation, sustainable development and awareness initiatives at the intersections of animals, people and the environment. Rohit is also co-Chair of Waterloo’s Toronto Alumni Chapter, our largest global alumni chapter, with over 50,000 alumni. In addition to his BSc in Health Studies & Gerontology from Waterloo, he holds a Doctor of Public Health (PhD) from the Johns Hopkins Bloomberg School of Public Health and a Masters of Public Health (MPH) in Global Health & Epidemiology from Boston University.
In relation to the COVID-19 response, and in collaboration with stakeholders like the World Health Organization, Coalition for Epidemic Preparedness Innovations, Bill & Melinda Gates Foundation, Novartis and others, Rohit is currently leading a study and advising an international consortium of donors, on the R&D systems in place for the development of global health products. This includes a review of the R&D processes around diagnostics, therapeutics and vaccines for poverty-related and neglected diseases, including for COVID-19. His team is also in the process of developing a platform for tracking the unprecedented innovation arising from the current pandemic.

Read more
Alumni, faculty, staff and community contributors are among this year’s winners and nominees, highlighting Waterloo’s impact across sectors

Read more
Waterloo researchers and frontline health partners receive $250,000 from the Graham Seed Fund to guide responsible AI adoption in real-world care settings

Three people walking in a public park. (Getty Images/FG Trade)
Read more
Subtle differences in speed, step length and rhythm could offer a low-cost tool for improving diagnosis at the earliest stages of neurodegeneration
The University of Waterloo acknowledges that much of our work takes place on the traditional territory of the Neutral, Anishinaabeg, and Haudenosaunee peoples. Our main campus is situated on the Haldimand Tract, the land granted to the Six Nations that includes six miles on each side of the Grand River. Our active work toward reconciliation takes place across our campuses through research, learning, teaching, and community building, and is co-ordinated within the Office of Indigenous Relations.