
Meet three Pharmacy alumni on the front lines
From neighbourhood pharmacies to community health teams, these Warriors are doing their part to keep us healthy

From neighbourhood pharmacies to community health teams, these Warriors are doing their part to keep us healthy
By Alana Rigby School of PharmacyCOVID-19 has impacted health-care systems worldwide. Pharmacies provide an essential service, ensuring that people can access medications and health information.
From neighbourhood pharmacies to community health teams, alumni from the School of Pharmacy have risen to the challenge, working hard through the pandemic to keep our world healthy. Here are a few of their stories.
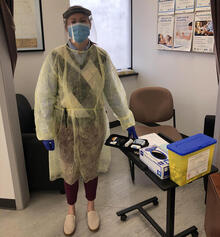 Dani Thomas (PharmD ‘18) stands a good distance from a car in the parking lot of Two Rivers Family Health Team in Cambridge. The person inside has their window rolled down and Dani’s wearing a mask, asking them questions. It’s mid-May and still snowing.
Dani Thomas (PharmD ‘18) stands a good distance from a car in the parking lot of Two Rivers Family Health Team in Cambridge. The person inside has their window rolled down and Dani’s wearing a mask, asking them questions. It’s mid-May and still snowing.
The person in the car is one of family health team’s patients on warfarin, a blood thinning medication that requires regular and careful monitoring by a pharmacist. Dani, a pharmacist on the team, jots down notes from the discussion and takes a drop of blood from the patient’s finger to test their levels.
This drive-thru method is a new way to administer medicine and check-in on patients while many health offices remain closed for walk-in appointments. At the family health team, Dani is one of many health professionals who collaborate to support their roster of patients.
“While the clinic doors have been opened to a few more patients, I am continuing to see and monitor patients from their vehicles as we still want to limit the number of patients entering the building as much as possible,” she says. “July was very hot out there in full PPE but to keep my patients safe is always a priority. We are in the midst of planning to restart clinics that have been put on hold such as memory clinic, so it will be interesting to see how the next few months unfold.”
Through it all, Dani’s patients have been supportive and understanding.
“It has truly been a team effort managing COVID-19,” she reflects. “Every single discipline in our team has been vital and we’ve really come together to help our patients. The changes in workflow took some adjusting to on my part, but it’s becoming familiar now. It’s also been inspiring to see how the community has united at this time – people dropping off supplies and little things like ear-savers to help us with wearing masks, showing thanks to their frontline workers.”
 Fatimah Jaffer (PharmD ‘15) remembers a conversation with coworkers in February. They were discussing one of the first COVID-19 patients admitted to the Royal Free Hospital in Hampstead, North London, England.
Fatimah Jaffer (PharmD ‘15) remembers a conversation with coworkers in February. They were discussing one of the first COVID-19 patients admitted to the Royal Free Hospital in Hampstead, North London, England.
“One of the doctors asked a senior pharmacist what blood work he should monitor for a patient who tested positive for COVID,” she says. “The pharmacist said she didn’t know. And how could she? No one knew anything about this new virus. One week, we were avoiding ibuprofen and a few weeks later it was being investigated as a treatment option.”
In England, where Fatimah has worked as a pharmacist since 2019, COVID-19 hit harder and faster than in Canada. The United Kingdom has a much higher population on a much smaller land mass, and this combination gave the virus ample opportunity to run rampant. As of early June, the country has seen over 40,000 deaths from COVID-19. Fatimah went from being responsible for 15 patients a day to 60 patients a day during the peak.
FATIMAH JAFFER, Alumnus and pharmacist
I went home every day knowing that I did the best I could given the information and resources I had. It was sink or swim, and we had no choice but to swim.
“The team spirit through all of this kept me going,” Fatimah says. “We’re in it together, trying to survive and safely care for and discharge as many patients as we can. I went home every day knowing that I did the best I could given the information and resources I had. It was sink or swim, and we had no choice but to swim.”
Today, the hospital is adapting to what caseloads allow, returning staff to normal working hours and re-starting some elective surgeries.
 When COVID-19 first hit Canada, Brad Murphy’s (PharmD ‘19) job at the Children’s Hospital of Eastern Ontario in Ottawa continued as normal. As a research pharmacist, he supports projects in pharmacogenomics — using an individual’s genetic markers to make decisions about their medications — in oncology and mental health, and he was able to keep working with little disruption.
When COVID-19 first hit Canada, Brad Murphy’s (PharmD ‘19) job at the Children’s Hospital of Eastern Ontario in Ottawa continued as normal. As a research pharmacist, he supports projects in pharmacogenomics — using an individual’s genetic markers to make decisions about their medications — in oncology and mental health, and he was able to keep working with little disruption.
But then Brad’s director put out a call for help. Some long-term care (LTC) homes in the Ottawa area had been devastated by COVID-19, experiencing cases among both residents and staff. COVID-19 caused the needs of residents to escalate and the demand for care surpassed what existing staff could provide, especially with some employees in quarantine due to testing positive. The LTC facilities were seeking volunteers to help continue to care for residents.
“I had more flexibility because of my work,” Brad says. “So, I decided to volunteer. Because I’m volunteering with patients who are COVID positive, I’m no longer allowed back in the hospital, so my research work is continuing from home.”
BRAD MURPHY, Alumnus and frontline volunteer
Doing this work has shown me a whole new side of health care.
As a volunteer Care Support Assistant, Brad supports the nurses, personal support workers, and residents, bringing meals, doing laundry and talking to residents. It’s heart-wrenching work at times. The conversations are sometimes stilted, but Brad does what he can, assisting with feeding residents and trying to answer their questions.
“Being in the homes has definitely pushed out the edges of my comfort zone,” Brad says. “But I had to help. I pictured if it was my grandparents and if they were going without being fed or bathed or socialized with, I would hope someone else would step up to the plate to help them. Doing this work has shown me a whole new side of health care.”

Read more
New evidence-based classification rules expand access and improve fairness for Para Cross Country and Para Alpine skiers

Read more
Waterloo Pharmacy alum spearheads outpatient oncology clinic for patients undergoing cancer treatment at WRHN

Read more
And a new model for how quantum research is shared — opening doors for the next generation of scientists and entrepreneurs
The University of Waterloo acknowledges that much of our work takes place on the traditional territory of the Neutral, Anishinaabeg, and Haudenosaunee peoples. Our main campus is situated on the Haldimand Tract, the land granted to the Six Nations that includes six miles on each side of the Grand River. Our active work toward reconciliation takes place across our campuses through research, learning, teaching, and community building, and is co-ordinated within the Office of Indigenous Relations.