
Disinfection can help in efforts to recycle personal protective equipment
New disinfection method could allow PPE to be reused

New disinfection method could allow PPE to be reused
By Media RelationsHealthcare workers on the front lines of the COVID-19 pandemic could reuse personal protective equipment (PPE) up to five times, if necessary, using a two-step disinfection method.
The simple system, proposed by researchers in Canada and New Zealand in a study that has not yet been peer reviewed, combines storage for at least four days and treatment with either ultraviolet (UV) light, dry heat or chemicals to kill coronavirus.
The system can be used on masks, gowns and other kinds of PPE now in short supply around the world.
“We identified useful disinfection methods that could be implemented quickly - in weeks or even days,” said Bill Anderson, an engineering professor at the University of Waterloo. “New PPE is always going to be better, but this two-step approach would be highly effective if reuse was necessary.”
José Derraik, a researcher at the Liggins Institute at the University of Auckland, said researchers examined studies from the SARS outbreak between 2002 and 2004 to help develop the process “because of the near absence of evidence on SARS-CoV-2, which is the virus that causes COVID-19.”
In step one of their proposed disinfection system, visibly soiled PPE would be discarded, while the rest was stored for at least four days to allow for the natural death, or deactivation, of the virus over time.
The most physically fragile equipment, such as N95 respirators, would then be treated with UV light to kill any remaining virus.
Depending on what they are made of, goggles, visors, gowns and masks would be subject to either heat, which accelerates the natural death of the virus, or a chemical disinfectant such as diluted bleach.
“Instead of relying on a single method, we would use time and its natural disinfecting effect, plus a more aggressive treatment approach to finish off the process,” said Anderson, a professor of chemical engineering.
Given the urgency of the crisis and the ongoing shortage of PPE, the researchers suggest their system could be implemented in hospitals and other facilities as soon as possible, then studied further while in use.
Anderson and Derraik collaborated with New Zealand doctors Elisabeth Connelly and Yvonne Anderson.
A paper outlining their proposed disinfection system, Rapid evidence summary on SARS-CoV-2 survivorship and disinfection, and a reusable PPE protocol using a double-hit process, appears online.
Note: This research has not yet been peer-reviewed and is being released as part of UWaterloo’s commitment to help inform Canada’s COVID-19 response.
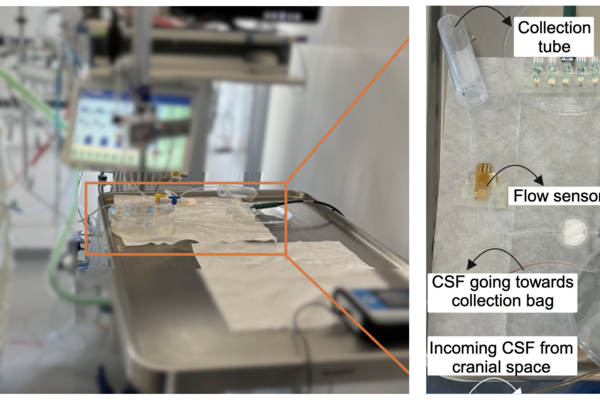
NeuroSense, a new bedside monitoring system designed to detect infections in brain-injured patients, being tested in an ICU setting (University Medicine Rostock).
Read more
New monitoring system tracks cerebrospinal fluid at the bedside for faster intervention

Read more
University of Waterloo researchers find arm slot and torso tilt play key roles in UCL strain

Read more
This year’s list spotlights nearly 100 innovators helping to strengthen Canadian sovereignty
The University of Waterloo acknowledges that much of our work takes place on the traditional territory of the Neutral, Anishinaabeg, and Haudenosaunee peoples. Our main campus is situated on the Haldimand Tract, the land granted to the Six Nations that includes six miles on each side of the Grand River. Our active work toward reconciliation takes place across our campuses through research, learning, teaching, and community building, and is co-ordinated within the Office of Indigenous Relations.